
We’re changing how we regulate to improve care for everyone.
What we’ve learned from the past five years puts us in a better position for the future. Our new strategy combines this learning and experience and we’ve developed it with valuable contributions from the public, service providers and all our partners. It means our regulation will be more relevant to the way care is now delivered, more flexible to manage risk and uncertainty, and will enable us to respond in a quicker and more proportionate way as the health and care environment continues to evolve.
This new strategy strengthens our commitment to deliver our purpose: to ensure health and care services provide people with safe, effective, compassionate, high-quality care and to encourage those services to improve. Our strategy is purposefully ambitious, and to implement it we will need to work closely with others to make it a reality. We’ll review this strategy regularly so we can adapt to changes and be prepared for what the future holds.
Our purpose and our role as a regulator won’t change – but how we work will be different.
We set out our ambitions under four themes
- People and communities: Regulation that’s driven by people’s needs and experiences, focusing on what’s important to people and communities when they access, use and move between services
- Smarter regulation: Smarter, more dynamic and flexible regulation that provides up-to-date and high-quality information and ratings, easier ways of working with us and a more proportionate response
- Safety through learning: Regulating for stronger safety cultures across health and care, prioritising learning and improvement and collaborating to value everyone’s perspectives
- Accelerating improvement: Enabling health and care services and local systems to access support to help improve the quality of care where it’s needed most
Core ambitions
Running through each theme are two core ambitions:
- Assessing local systems: Providing independent assurance to the public of the quality of care in their area
- Tackling inequalities in health and care: Pushing for equality of access, experiences and outcomes from health and social care services
We’ll look at how the care provided in a local system is improving outcomes for people and reducing inequalities in their care. This means looking at how services are working together within an integrated system, as well as how systems are performing as a whole.
We’re committed to our ambition of regulating to advance equality and protect people’s Human Rights. Everyone in health and social care has a role to play in tackling the inequalities in health and care for some people. This strategy sets out our ambition for how we can help influence change.

People and communities
We want to be an advocate for change, with our regulation driven by people’s needs and their experiences of health and care services, rather than how providers want to deliver them.
This means focusing on what matters to the public, and to local communities, when they access, use and move between services. Working in partnership with people who use services, we have an opportunity to help build care around the person: we want to regulate to make that happen.
Listening and acting
People need to see how their voice can make a difference to the safety and quality of the services they use and how we reflect their experience in our work. We want to hear both positive and negative experiences when people access, use and move between services.
- We’ll make it easier for people, their families and advocates to give feedback in the most convenient and suitable ways for them whenever they want. We’ll also enable those who act as trusted intermediaries to share feedback with us. Working with local communities, we’ll make the most of existing sources of feedback so people don’t have to repeat themselves.
- We’ll identify more and better ways to gather experiences from a wider range of people and develop the skills and tools that we need to do this. We’ll reach out to people whose voices and experiences we don’t often hear: people who are the most disadvantaged in our society, have had distressing or traumatic experiences, and those who are more likely to experience poor outcomes and inequalities. This includes people with a learning disability, people with communication needs, people living in poverty, those whose voices are not often heard, those who are detained under the Mental Health Act, and people who are at risk of abuse or other human rights breaches.
- A priority will be improving our capacity and capability to get the most out of feedback. We’ll change the way we record and analyse people’s feedback so it’s easier for us to quickly identify changes in the quality of care – both good and bad. We’ll be clear about the value and weight we give to quantitative and qualitative information when using it with other evidence.
People’s feedback is vitally important. It’s important to build trust with the public and motivate people to share their experiences.
- When we publish information about quality, we’ll be clearer about how we’ve used what people have told us – both good and bad. We’ll explain what action we and others have taken as a result.
- When people take the time to share their experiences with us we’ll provide a response in the way people need it and explain how their feedback has informed our view of quality.
People are often afraid to speak up. We want to help build a new culture among the public, health and care providers, and all our partners, that welcomes, values and acts on feedback.
- We’ll improve the way we assess how services and local systems encourage and enable people to speak up, and how they act on this feedback. It will be unacceptable if they are not doing this – where they are not, we will make sure they take action to address it. We’ll also focus on this when we look at how local systems are listening to their communities. This is so they can improve access to services that meet people’s needs, in particular people who are most likely to have a poorer experience of care or who are less able to speak up.
People are empowered
We know care is better when it’s developed through the eyes of people who use services and delivered in partnership with them. We think the same of regulation. When we talk about the quality of care in our work we will have people at the centre.
- To empower people to drive change, it’s important for them to know who we are and understand what we do. We’ll proactively raise public awareness of CQC and be clear about our role as a regulator. We’ll invest in the most effective ways to reach different groups of people.
- We’ll work closely with people who use services and those that represent them to understand their needs, and to co-design and develop how we work and our services for the public. Any changes we make will start with understanding what people expect and need from care services and pathways, and from CQC. We’ll involve people in a more equitable, targeted and meaningful way and enable them to engage with us in ways that best suit them.
- We’ll work with all our partners and people who use services to develop an agreed and shared view of quality that makes clear what standards people can expect from their health and care services. We’ll provide a clearer definition of what good and outstanding care looks like for everybody, based on people’s lived experience of care and what matters to them. Everybody will be able to easily access, understand, and use these definitions. We’ll use them as the basis for assessing services and the information that we collect as evidence. This shared view of quality will enable a joined-up approach that’s applied to individual services, corporate providers, and across system boundaries in health and social care.
Providing independent, trusted and high-quality information about the quality of care is a fundamental part of our work.
- We’ll change how we provide information so that it’s more relevant, up to date, and meaningful for people who use services, and reflects their experiences. We’ll ensure people have easy access to information in the way they need it, and use clear and accessible language.
- We’ll encourage people to use our information in ways that are relevant to them. Our up-to-date view of the quality of care in a service will help people and their families make informed decisions, where they can, about where to go for their care. It will also give people confidence that our information reflects the quality of care that they can expect.
Prioritising people and communities
- We’ll look at how effectively a service works with others, and in partnership with local communities, to involve people in designing and improving services. This includes how services embed equality, diversity and inclusion, and corporate social responsibility in everything they do, such as improving local health and wellbeing, and environmental sustainability.
Working collaboratively as a local system is essential to improving the quality and safety of care. Health and care services and commissioners need to understand the diverse needs of their local populations and where there are inequalities in how people access and experience care, and in their outcomes.
- When assessing individual health and care services, we’ll look at how they work together in an area, as one system, to deliver better and more coordinated care. We’ll focus on how well local systems perform against the important things that matter to people in that community – such as being able to move easily between services. We’ll work to build our understanding of the needs of a local population so we can hold services to account effectively.
Our work in this area will be through legislation in the Health and Social Care Bill and we’ll align with other regulators to encourage a shift towards more integrated services.
- Our assessments of local systems will provide independent assurance to the public of how they are working together to deliver high-quality care. We’ll ensure our people have the right skills and capability to assess at both a service provider and a system level.
- We’ll publish what we find about the performance of a system. If we see good practice, we’ll highlight this and share examples so that others can learn from it and adapt it to their own area. We’ll also make recommendations to improve where we find issues or concerns.
We will identify and call out unwarranted variation and inequalities in how people experience health and care services. But we also know that a person’s health and wellbeing is significantly affected by factors outside health and care.
- We’ll assess how local systems understand the needs of their local populations, especially people who face the most barriers to accessing good care and those with the poorest outcomes, enabling them to proactively address inequalities.
- We’ll work with other appropriate agencies, voluntary and community organisations, and other regulators to develop a shared understanding of the factors that contribute to inequalities in people’s access and experiences and how this affects their outcomes from using care services. Together, we’ll identify the levers that we can all use to tackle these inequalities.

Smarter regulation
We will be smarter in how we regulate. We’ll keep pace with changes in health and care, providing up-to-date, high-quality information and ratings for the public, providers and all our partners.
We’ll regulate in a more dynamic and flexible way so that we can adapt to the future changes that we can anticipate – as well as those we can’t. Smarter use of data means we’ll target our resources where we can have the greatest impact, focusing on risk and where care is poor, to ensure we’re an effective, proportionate and efficient regulator.
We have a baseline understanding of quality across health and social care. But we know that the quality of care can vary from day to day. We’ll use our regulatory powers in a smarter, more proportionate and consistent way to make the right decisions and take the right action.
- Our assessments of quality will be different. On-site inspections are a vital part of our performance assessments and essential to observe the care people receive. But they are not the only way to assess quality: we want to move away from relying on a set schedule of inspections to a more flexible, targeted approach. To do this, we’ll use all our regulatory methods, tools and techniques to assess quality.
- We’ll build stronger relationships with services and with local systems. This includes having ongoing conversations about quality, which will give us a better insight and enable us to tailor our approach to be more proportionate.
- We’ll visit when there’s a clear need to do so. For example, this could be when we’re responding to risk, where we only have limited data or we need specific information, where we need to speak to people using the service face-to-face, or to ensure that our view of quality is reliable. For some types of service, we’ll need to visit more often to observe care. Our continuous insight and monitoring activity mean that rather than spending time looking at paperwork when we’re on site, we’ll be able to make the most of our time – we’ll have better conversations with people who live in or use the service, and their families and advocates, and more time to talk with staff.
- We’ll build digital platforms that will better integrate the data we hold, which will enable us to interpret data in a more consistent way. We’ll use innovative analysis, artificial intelligence and data science techniques proactively to support robust and proportionate decision-making, based on the best information available.
Our ratings will be more dynamic – we’ll update them when there is evidence that shows a change in quality. We won’t always need to carry out an inspection to do this.
- Ratings will evolve to reflect how people experience care so they’re more meaningful and focus on things that matter to them. We’ll be clear about what information we use and how we use it in our judgements and decisions about ratings.
We all have a common drive to improve people’s care. From the point of registration, we’ll develop ongoing, collaborative relationships with services, built on openness and trust. We want this to enable effective and proportionate regulation so we can focus our work where quality needs to improve and minimise any unnecessary workload.
- We’ll work with service providers and other regulators and partners to coordinate data collections. To reduce the duplication and workload for services in collecting and submitting data to us, and to other organisations, we’ll only ask for the information we need and that we can’t get elsewhere. We’ll use information from other sources and share the information we gather ourselves through data-sharing agreements. We’ll collect data once and use it many times. We want this to help staff to focus on providing care safely and finding opportunities to improve.
- We’ll improve the way we connect with services digitally. Starting from the point of registration, where we do need to collect information directly we will make it easier for services to give us the information we need and simpler to update what they’ve already told us. We’ll also make it easier for services to access more of the information we hold about them by having it in one place.
We want everyone we work with to benefit from our regulation. The way we regulate will become more constructive and supportive – using what we know to help services to tackle problems early and providing up-to-date, high-quality information and ratings.
- We’ll share the data and information we hold on services with organisations that represent or act on behalf of people who use services, and with our partners and others where it will help them in their own work to improve people’s care.
Like the services we regulate, we’re evolving and adapting to changing models of care, such as integrated care systems and digitally-enabled care. The move to looking at how services work together in a local system is a change in our approach that better reflects how people experience care – we think this is a smarter way to regulate.
- We’ll work with service providers, partners and other regulators to align our activity, understand how care is changing and ensure that our regulatory model keeps pace with changes.
- By improving the way we register services, we’ll be better able to hold organisations to account for people’s care. We’ll expand our definition of what we consider to be a provider of care and what it means to carry on a regulated activity. This will make sure that we register all the parts of an organisation that are responsible for directing or controlling care; and importantly, this will make sure they can be held accountable.
- Our assessments will always focus on what matters to people as they access, use, and move between services. We’ll also look more closely at aspects that we know have a positive effect on quality such as the culture of a service, how it works with other services in a local system, and how it drives improvement.
- We’ll focus our assessments on how services and local systems are working to ensure equal and appropriate access to good health and care services for everyone. The information we gather will enable us to better understand the risks of inequalities in people’s experiences of their pathway through care and their outcomes. We’ll take action where we see a need for improvement.
We want our ratings and information to help people to make informed choices about their care, and to give services an assessment of their quality to encourage them to improve.
- We’ll use our clearer definition of quality as a reference for what good and poor care looks like. We’ll explain clearly how we use this to assess the quality of services and how we decide what information to collect as evidence. This definition will be at the heart of our regulatory processes and will help us improve consistency in what we do – so people can be confident that good means good wherever they are in the country and whichever service they are using.
- We’ll move away from long reports written after inspections, and instead provide information and data to better meet the needs of all audiences, including people who use services. Information will be easier to understand and more accessible. We want people to be able to get information in ways that suit them.

Safety through learning
We want all services to have stronger safety and learning cultures. Health and care staff work hard every day to make sure people’s care is safe. Despite this, safety is still a key concern for us as it’s consistently the poorest area of performance in our assessments.
It’s time to prioritise safety: creating stronger safety cultures, focusing on learning, improving expertise, listening and acting on people’s experiences, and taking clear and proactive action when safety doesn't improve.
Having the right organisational culture is crucial to improving safety. This means safety must be a top priority for all – regardless of seniority or role. A strong safety culture needs everyone working in health and care, as well as people who use services, to play their part. In a strong safety culture, risks aren’t overlooked, ignored, or hidden – and staff can report concerns openly and honestly, confident that they won’t be blamed.
- We’ll work with others to agree and establish a definition and language about safety and how this could apply in different health and care services. This will create a better understanding of risk across all health and care – so that we all know what’s not acceptable – and therefore help to reduce avoidable harm, neglect, abuse and breaches of human rights. When we talk about safety we’ll make sure it reflects what’s most important to people when they use services. More clarity will enable services to prioritise the essentials and have clearer expectations when we assess them.
- We’ll be looking for cultures that have learning and improvement at their core. In a good safety culture, it’s accepted that all incidents – positive, negative, or wholly avoidable – provide opportunities to learn and improve. It’s important that we also embody a learning culture and demonstrate this in our relationships with providers and all our work.
- Our assessments of safety will have a sharper focus on checking for open and honest cultures. We’ll encourage health and care staff to speak up about safety issues where they work, including where there may be safeguarding issues. We’ll expect all services to have stronger safety and learning cultures and that learning, and improvement should be the primary response when anyone speaks up. We want staff to feel confident that we’ll also listen and act when they raise concerns with us, and we’ll intervene quickly where appropriate.
- We can do more to help services improve safety by sharing the insights, learning, and exemplary practices that we’ve identified. We’ll use our independent voice to highlight the changes and improvement that services have made to improve safety as a direct result of our regulatory actions.
Knowledge is crucial to having the right safety cultures, but there are different levels of knowledge and expertise in different types of service and sectors.
- We’ll look at how services and systems assure themselves that they have the right knowledge and expertise, and how they are investing in improving safety.
- We’ll improve and increase our own safety expertise in CQC to ensure our approach is in line with the latest safety thinking. Together with our unique data and insight, this will enable us to challenge and highlight failures in services and in systems.
People should be able to influence the planning and prioritisation of safe care and be truly involved as equal partners in their care at all levels. This collaborative approach has the potential to transform safety and to ensure that people’s human rights are upheld.
- In our assessments we’ll look for processes to show that leaders and staff are committed to involving people in their own safety throughout their health and care journey, and the impact this has on their outcomes. We’ll check that services actively take into account people’s rights and their unique perspectives on what matters to them in the way they choose to live their lives and manage risk. This includes having the information they need to help them be equal partners in their care and play a part in their own safety.
We know that some of the greatest safety risks – both physical and psychological – happen when people struggle to access the right care, when they’re transferred between services or after they’re discharged. We also know that some services are more likely to have greater safety risks than others.
- We’ll review how effectively we are assessing and monitoring safety – from registration through to enforcement. We’ll use our improved safety expertise to make sure we’re taking the right approach. As part of this, we’ll review how we gather data to ensure greater consistency across sectors regardless of who it is reported to.
- Learning and improvement must be the primary response to all safety concerns in all types of service and local systems. Where we have concerns, we will direct services and systems to respond and show us – and people who use the services – what action they’ll take to learn and improve. We’ll share this information with the public as part of our up-to-date view of quality.
- Services that are not open to learning can’t be safe. We’ll use our powers and act quickly where improvement takes too long, or where the changes won’t be sustainable. We’ll take action where services are unable to identify systemic issues in their own organisational culture or fail to learn lessons from widely publicised failures happening across health and care.
- We’ll change how we regulate safety in all services to reflect new ways of delivering care and as more services work as part of a local system. We’ll check how well services work together – those that are truly focused on safety will be determined to ensure a safe journey of care for people moving on to a different service, or when being transferred between services for ongoing care.
- Where we see systemic safety issues in a local area, we’ll speak out to encourage meaningful change. We’ll share the learning from our insight on themes, trends, and best practice to help services and local systems improve their safety. We’ll also share with regional organisations our data and information about safety in local systems, to support their oversight of safety in their area.
To improve safety, service providers may need support and guidance. In some sectors, there’s a national team of experts who provide guidance and alerts about safety. But this type of national support and oversight doesn’t exist in all sectors.
- It’s crucial that all health and care services have consistent access to the right support and insight to help them build strong safety cultures, learn from safety and safeguarding incidents, and improve their practice. We’ll work with others to develop solutions to ensure that all services have support and leadership during difficult times, and that they have the right tools to always provide safe care. We’ll need to understand where this oversight is best placed and develop the right frameworks as needed.
- We’ll use our insight and independent voice to promote a national conversation on safety across health and care sectors and systems. We can use this to drive improvements in safety cultures and reduce harm.

Accelerating improvement
We will do more with what we know to drive improvements across individual services and systems of care. We’ll use our unique position to spotlight the priority areas that need to improve and enable access to support where it’s needed most.
We’ll empower services to help themselves, while retaining our strong regulatory role. The key to this is by collaborating and strengthening our relationships with services, the people who use them, and our partners across health and care.
The support that’s available to improve the quality of care varies between and within health and care sectors and across England. We’ll work collaboratively to support all parts of a local system to focus on improvement.
- Where there are gaps in improvement support, we will facilitate national improvement coalitions with a broad spectrum of partners within both health and adult social care, including those representing people who use services. These coalitions will work collaboratively to improve the availability of support, both nationally and at a local system level. This will build on existing partnerships and programmes around improvement rather than duplicate efforts. We’ll champion consistent access to direct, tailored, hands-on support for all services who need it.
- Local systems need to drive improvement in their areas. We will support these efforts and assess how well they are doing this, including how well they are ensuring everybody has fair and equal access to care, an equally good experience and good outcomes. We’ll strengthen our ongoing relationships at a local level to promote collaboration on improvement across areas, working with local and national partners from the relevant improvement coalitions.
We want to see improvements that benefit people. We’ll play an active part in this by setting clear expectations and empowering services and local systems. But we’re clear that while enabling access to support, we will retain our core regulatory role, which means using our powers to act where we see poor care.
- We’ll encourage continuous improvement in quality by being clearer on the standards that we, and people who use health and care services, expect. Services and local systems will need to demonstrate a culture of improvement and contribute to improvement in their local area. As part of this, we’ll expect them to address inequalities in access, experiences and outcomes.
- We’ll develop collaborative relationships with services, helping them to find their own route to improvement. This will involve facilitating access to improvement support and pointing services to sources of guidance, best practice, and other providers and organisations that can offer advice and support. We’ll hold improvement conversations with services and offer a range of resources to support them to decide for themselves the best way forward rather than telling them what to do. We will develop our skills, capability, and culture to enable this shift.
- In collaboration with others we'll identify the areas that need to improve as a priority – both at a local and national level. Using our independent voice, we’ll deliver a programme of activity to drive change in these areas, based on evidence of what works. We’ll share good practice and examples of the factors that drive improvement, and the findings from our in-depth reviews. We’ll prompt action through events and workshops, and by publishing guidance, tools, and frameworks that support improvement.
- We’ll empower services and local systems to improve themselves by offering analysis and benchmarking data. This will enable them to self-assess how they’re performing against similar services and areas. Our benchmarking information will also show us where we need to focus our work to drive improvement.
Innovative practice and technological change present an opportunity for rapid improvement in health and care. We have a role in creating a culture where innovation and research can flourish.
- We’ll encourage and champion innovation and technology-enabled services where they benefit people and where the innovation results in more effective and efficient services. We know the path to innovation can be difficult; we want to use what we know as a regulator to create an environment where services can try new ways to deliver safe, high-quality care. We’ll aim to support their efforts to innovate through clear advice and guidance.
- We’ll understand and keep pace with changes, both in new technology and new ways to deliver care. We’ll work in partnership with services and other stakeholders to develop a coordinated, effective, and proportionate approach to regulating new innovations and technology. When we do this, we’ll consider where the use of new technology to deliver care might not suit some people, and what services need to do to make sure that nobody is disadvantaged.
- Research can help improve the quality of care, and people often value the opportunity to participate in research, whether clinical trials or other studies. We’ll encourage services to play an active part in research to improve care for all, foster innovation and enhance people’s experiences of care.
We have valuable knowledge and insight about improvement – we’ll use this to inform our regulatory approach.
- We want to promote an improvement culture across health and social care. Through our assessments of services and local systems, and across all our work, we’ll identify and investigate the things that are most important to ensuring good quality care. We’ll use the evidence we collect to support improvement.
- We’ll invest in research and make better use of external evidence to have a better understanding of the conditions that drive quality improvement, including evidence and best practice from other industries. We will also strengthen our evidence on the extent and nature of inequality in people’s experiences of care, and the good practice to help reduce this.
- We’ll use the best available evidence to inform our approach to regulation. We’ll develop and extend our own internal improvement activity and capability. As part of this we will embed a culture of learning and evaluation in CQC to maximise our impact on the quality and outcomes of care for people.
Outcomes from this strategy
Our strategy on a page
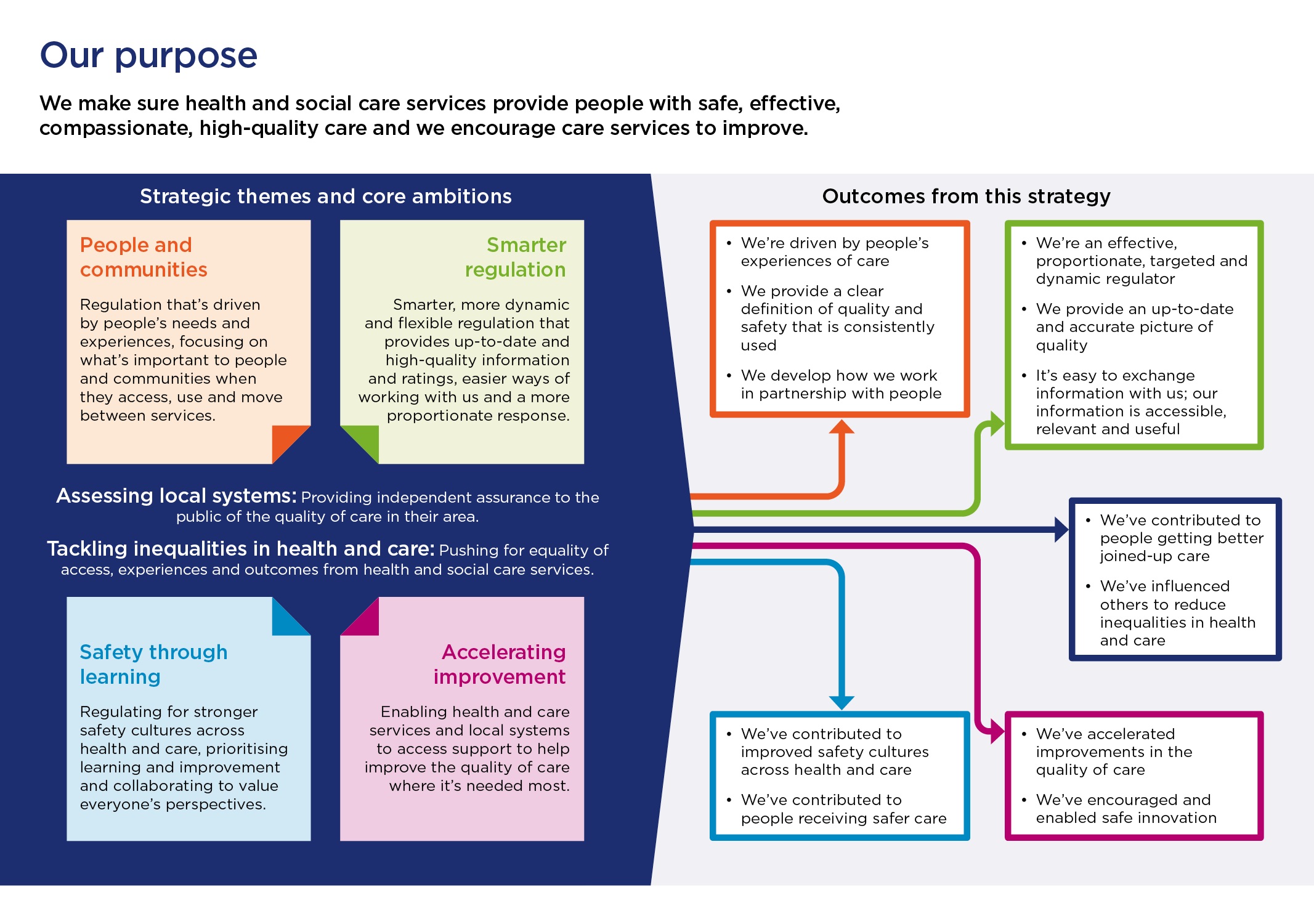
By delivering this strategy, we will achieve 12 outcomes:
People and communities outcomes
- Our activity is driven by people's experiences of care.
- We clearly define quality and safety in line with people’s changing needs and expectations. This definition is used consistently by all people, and at all levels of the health and social care system.
- Our ways of working meet people’s needs because they are developed in partnership with them.
Smarter regulation outcomes
- We are an effective, proportionate, targeted, and dynamic regulator.
- We provide an up-to-date and accurate picture of quality.
- It is easy for health and care services, the people who use them and stakeholders to exchange relevant information with us, and the information we provide is accessible, relevant, and useful.
Safety through learning outcomes
- There is improvement in safety cultures across health and care services and local systems that benefit people because of our contribution.
- People receive safer care when using and moving between health and social care services because of our contribution.
Accelerating improvement outcomes
- We have accelerated improvements in the quality of care.
- We have encouraged and enabled safe innovation that benefits people or results in more effective and efficient services.
Core ambitions: Assessing health and social care systems, and tackling inequalities in health and social care
- We have contributed to an improvement in people receiving joined-up care.
- We have influenced others to reduce inequalities in people’s access, experiences and outcomes when using health and social care services.